An interventional pain management specialist with EmergeOrtho in Wilmington, Ruth Anderson, MD, wants people who suffer from chronic severe headaches to know that relief is not only possible, it’s highly probable—and without taking narcotics.
“Pain management physicians bring a unique approach to treating migraine headaches,” explained Dr. Anderson. “Many times, migraine headaches can be treated with interventional procedures to help limit the amount of medication a patient needs to take and improve the effectiveness of the medications they do take.” Not only does this approach limit side effects, continued Dr. Anderson, it also prevents what’s known as rebound headaches or medication overuse headaches.
“After a period of time, the medications can cause the headaches to become more frequent and difficult to treat,” she said. “When that happens, the only way to treat the rebound headaches is to have the patient detox off the pain medications that caused the problem.”
Dr. Anderson explained that while many people use the term migraine for any bad headache, a classic migraine is unilateral, or only on one side of the head. “But whether it is a real migraine or another form of headache it doesn’t matter,” she emphasized. “If it’s a terrible headache, it needs to be treated, regardless of what it’s called.”
In place of narcotics, Dr. Anderson uses a variety of interventional procedures to treat headaches, including Botox, sphenopalatine ganglion (SPG) blocks, facet joint injections and occipital nerve blocks. “The more I can use these treatments, the fewer medications my patients will need and the better quality of life I will help them maintain,” she said.
Botox
OnabotulinumtoxinA or Botox, the same treatment used to treat facial wrinkles, has been successful in treating migraine headaches. Physicians believe that Botox works by blocking neurotransmitters that carry pain signals from the brain to the nerve endings in the head and neck. Botox injections interrupt that transmission, thereby preventing the pain.
It’s important to note that Botox is approved for use in adults who get chronic migraines, but not for occasional migraines nor for other types of headaches.
SPG Blocks
Another very successful treatment option for migraine headaches, as well as trigeminal neuralgia, is called sphenopalatine ganglion (SPG) block, explains Dr. Anderson. Trigeminal neuralgia is a severe face pain that can be incapacitating, even to the point of sufferers being unable to chew because of the pain.
In the skull, there are two ganglia (relay hubs of nerves) behind the bones of the face: the trigeminal ganglion and the sphenopalatine ganglion. “An SPG block involves putting a small, soft rubber tube up the nose and squirting a local anesthetic in the area of the sphenopalatine ganglion,” explained Dr. Anderson. “It sounds a bit unsettling, but it’s a simple,safe, in-office procedure that takes only a few minutes and is highly effective.”
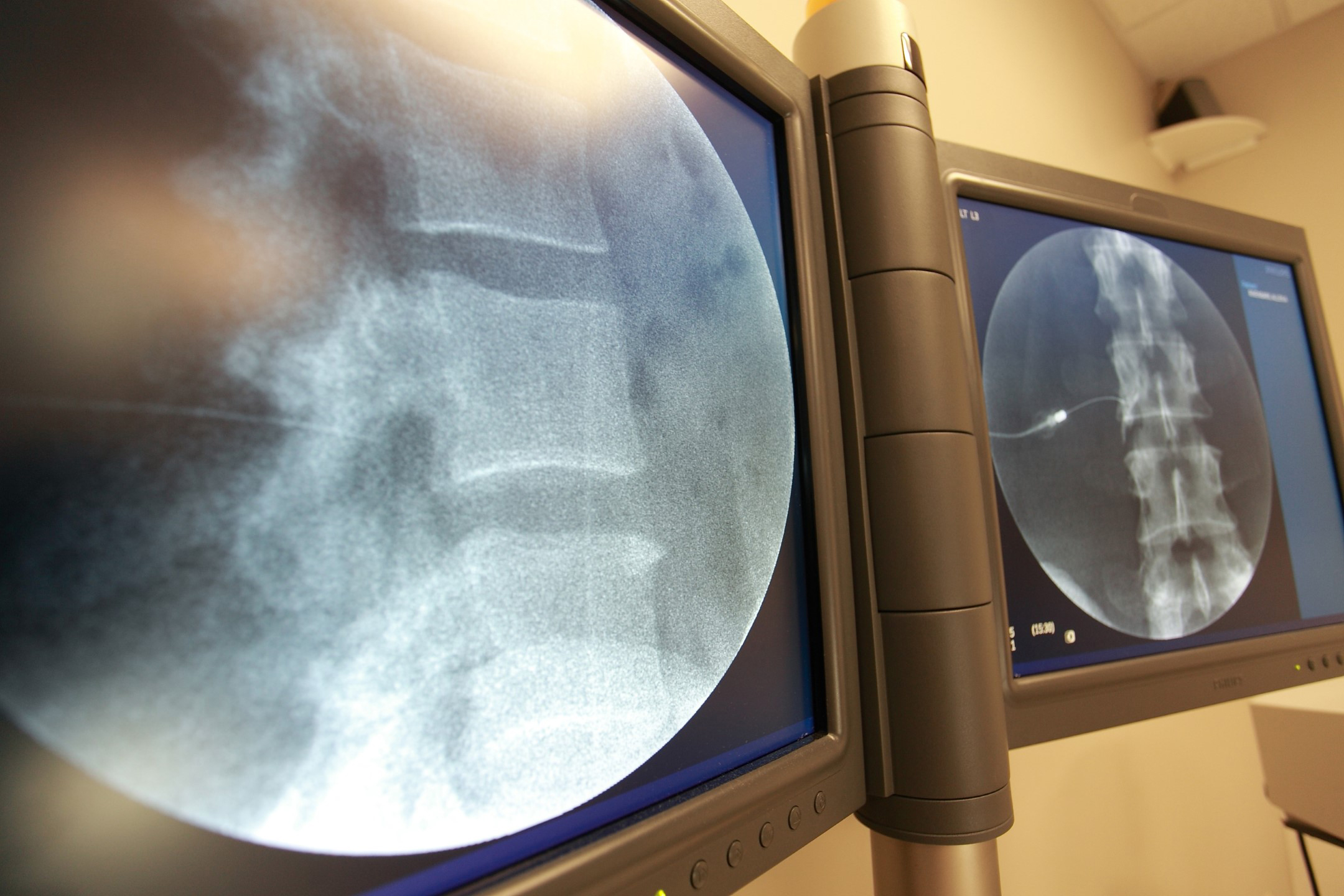
Cervical Injections
Other types of headaches that patients call migraines arise from the cervical spine—specifically the upper joints between the vertebrae, called facet joints, and the nerves at the base of the skull called occipital nerves. Called cervicogenic headaches, they are driven by arthritis and cause pain that can radiate over the top of the head or over the ears and even settle behind the eyes.
“I had a patient when I was practicing in California who was seeing an ophthalmologist for severe, chronic eye pain, but without success,” said Dr. Anderson. “He just felt his case was hopeless. However, through injections in the joints of the spine and occipital nerves, we were able to get him profound relief. He just couldn’t believe it. I never saw a bigger, toothless grin.”
These injections are only done by pain management specialists using a video Xray machine. “If this is the cause of your head and/or neck pain, there is a long-lasting procedure that can give significant relief for six months or longer,” said Dr. Anderson.
Avoiding Opioids
With all the publicity surrounding the opioid addiction crisis in the United States, many people avoid taking strong medications altogether.
“Sometimes patients tell me they didn’t want to see a pain management doctor because they don’t want to have to take narcotics,” said Dr. Anderson. “I tell them they came to the right place because I don’t prescribe them. Giving narcotics for any type of pain is always a last resort for me, never a first step. However, I will never give them for migraines. That policy is set in stone simply because narcotics are one of the leading causes of rebound or medication overuse headaches, so ultimately it will make them worse, not better.”
Dr. Anderson said while treating migraines was not initially part of her practice when she moved to Wilmington to join EmergeOrtho in 2017, she soon became aware of the need.
“I saw so many people who were being poorly treated or undertreated, and suffering with more than 15 headaches a month,” she said. “This part of my practice has grown significantly in recent years, all by word of mouth.”
To schedule a consultation with Dr. Anderson at either of the EmergeOrtho locations at 2716 Ashton Drive in Wilmington or 8115 Market Street in Porters Neck, please call EmergeOrtho at 910.332.3800.